Translate this page into:
The influence of uneven placement of mini dental implants on retention form of lower complete over denture: An in vitro study

*Corresponding author: Abdullah Alajmi, Department of Prosthodontics, Diwan of Royal Court Medical Services, Muscat, Oman. dr.alajmix@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Alajmi A, Roudsari R, Barclay C, Zeinalddin M. The influence of uneven placement of mini dental implants on retention form of lower complete over denture: An in vitro study. J Global Oral Health. doi: 10.25259/JGOH_1_2024
Abstract
Objectives:
This in vitro study aimed to evaluate the effect of placing two mini-dental implant (MDI) at different heights on the retention form of the lower over denture (OD).
Materials and Methods:
Sixteen acrylic mandibular blocks and their corresponding ODs were prepared and divided into four groups (four sets per group) to represent an atrophic mandibular ridge with two MDIs placed parallel to each other at inter-implant heights (IHs) of 0.0, 1.5, 3.0, and 4.5 mm. The OD blocks were mounted on a manual pulling stand and pulled vertically 12 times to measure the peak tension load (N). The data were analyzed using one-way analysis of variance (ANOVA), and the differences between the means were compared (P < 0.05).
Results:
One-way ANOVA showed a statistically significant effect of IH on the retention force of the OD blocks (P < 0.05). The mean retention force (N) for evenly placed MDIs was as follows: 32.2 ± 0.95, 1.5 mm IH: 30.1 ± 0.56, 3.0 mm IH: 26.1 ± 0.71, and 4.5 mm IH: 27.4 ± 0.90.
Conclusion:
The retention force of the OD blocks was significantly affected by the vertical inter-implant distance. A significant reduction in the mean retention force was observed for ODs retained by MDIs placed at an IH >1.5 mm.
Keywords
Mini-implants
Over denture
Prosthodontics
In vitro
INTRODUCTION
Patients who wear complete dentures (CDs) experience lower jaw resorption over time, leaving less bone to retain the lower denture in place. The rate of residual ridge resorption varies between individuals.[1,2] Patients with a history of cleft lip and palate, surgical excision of pathoses, traumatic injury,[3] or sequential loss of teeth over a long period[4] may show atrophic and uneven residual ridge. The literature shows that a denture wearer’s quality of life can be improved by providing the patient with two standard-size dental implants (SDIs) in the lower jaw to retain the mandibular over denture (OD) in place.[5,6] However, several factors could preclude this treatment modality from older patients, such as the patient’s age, existing medical conditions, quantity and quality of mandibular alveolar ridge, the invasive nature of placing SDIs, the need to use bone graft surgical procedures,[7] and uneven RR height. Over the past 20 years, mini-dental implants (MDIs) have evolved from temporarily retaining provisional prostheses to becoming established as a definitive, long-term treatment modality.[8] These findings increased the popularity of MDIs for managing atrophic mandibles.[7,9]
The purpose of this in vitro study was to investigate the effect of unevenly placed one-piece design MDIs with a ball attachment system on the retention form of the lower OD. The hypothesis was that the unevenly placed MDIs with ball attachment systems would not influence the retention form of the lower OD.
MATERIALS AND METHODS
The sample size was calculated using the G*Power software (version 3.1.9.6), which determined that a total sample size of 16 (n = 4 samples/group) would have a power of 80% to detect a difference in the means between groups, with an effect size f = 1.15 and a significance level of P ≤ 0.05[10] [Figure 1]. To determine the peak retentive values for each group, the mean of each specimen was calculated from the 12 vertical pulls. The overall mean for each of the four groups (0.0, 1.5, 3.0, and 4.5 mm) was determined by averaging the specimen means. In total, 32 MDIs (Southern Implants©, UK) were used along with cold-cure acrylic resin (Bracon Ltd, UK) to create the corresponding ridge and OD blocks (16 sets in total, four sets in each group). The MDIs (2.4 mm × 10 mm) were grade IV titanium, and the attachment housings were made of titanium alloy Titan Grade 5 ELI. The ball attachment had a diameter of 1.8 mm and was incorporated into the implant as a one-piece design. The MDIs, retentive caps, and metal housings were manufactured by Rhein83 (Italy) and all product specifications were obtained from Southern Implants©. Four wax blocks shaped into four different height levels 0.0, 1.5, 3.0, and 4.5 mm inter-implant height (IH) differences. The four wax blocks (42 × 22 × 22 mm) were prepared with inter-ridge heights of 0.0, 1.5, 3.0, and 4.5 mm. Oversized osteotomies were then prepared at inter-implant distances (ID) of 22 and 10 mm from the edges. In addition, cure silicone (Shera© Werkstoff Technologies, Germany) was mixed and poured into the osteotomies and square plastic bowls. IHs were verified using a ruler and an electronic digital caliper before and after implant placement. A screw hole of 6.0 mm diameter was drilled at a 90° angle to the block surface.
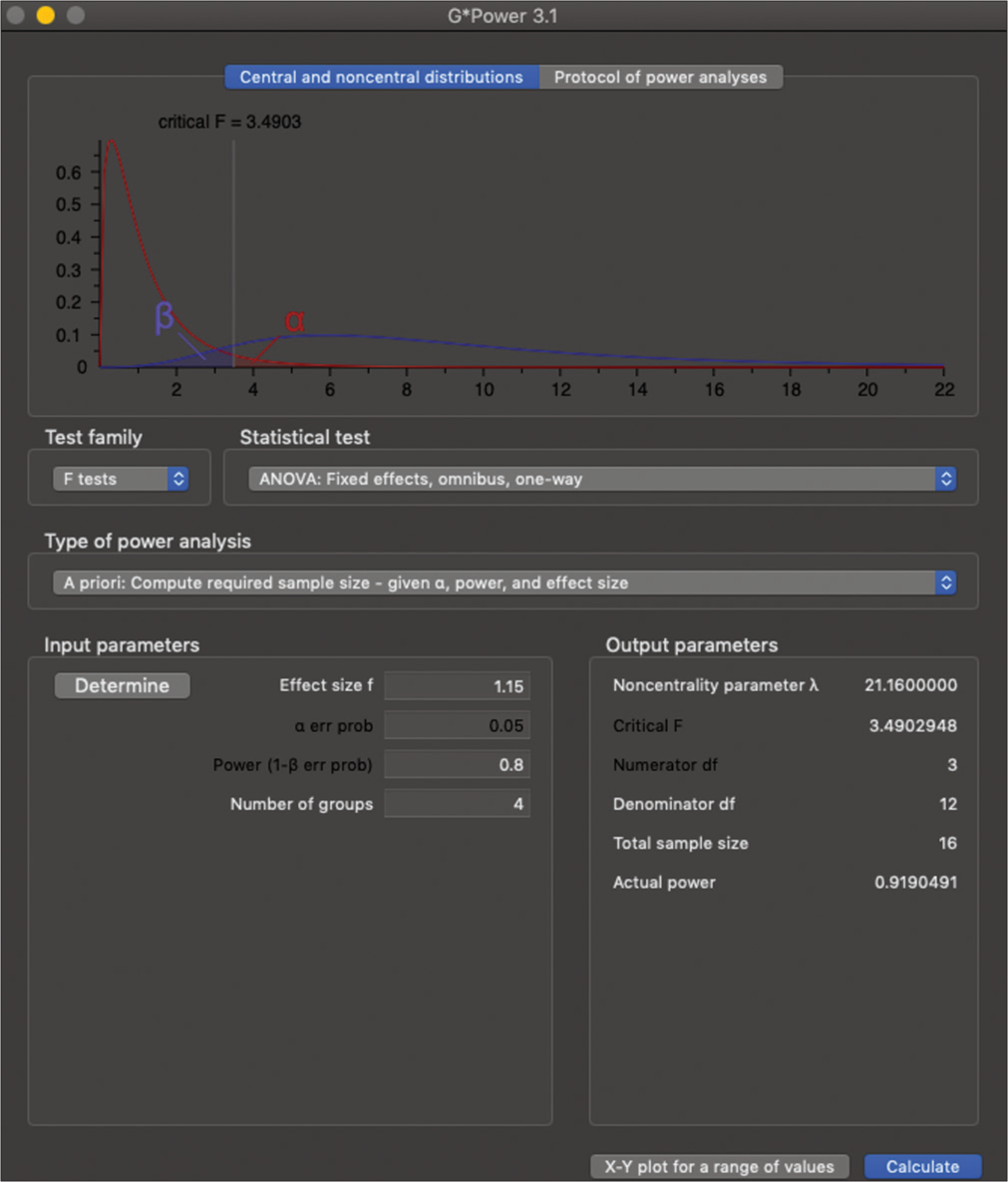
- Sample size calculation.
All acrylic blocks were polished using 120- and 220-grit sandpapers to remove any surface irregularities that could hinder the retention force. Four screw hooks were placed on each OD block 5 mm from the block edges. They were not drilled into the acrylic resin but were placed before the acrylic setting. The four hooks allowed four chains to have a rigid grip for each block. The centers of the engraved osteotomies in the wax blocks were placed 22 mm apart and 10 mm from the block edges. A cylindrical silicone mold is used to prepare a custom-made acrylic key to attach the MDI holder to the surveyor. Cold-cure acrylic resin was mixed and poured into the mold, allowing it to set under the surveyor with the analyzing rod in it. The MDI holder is attached to the acrylic key using incremental buildups of cold-cured acrylic resin. The MDIs were placed in oversized pre-prepared osteotomies using a surveyor to achieve parallelism and consistency. Each osteotomy was half-filled with cold-cure acrylic, which allowed the MDIs to attach firmly to the blocks, followed by additional acrylic to seal the osteotomy. Once the acrylic resin is set, the metal housings with standard retentive caps (retention force of 1.8 kg) are clipped to the ball attachment on the MDIs. The OD block is placed over the implant block to allow precise positioning of the metal housing. The separating medium (Vaseline®) kept the implant and OD blocks separate. Once the setting was completed, the acrylic blocks were separated twice, vertically, to further inspect for any acrylic irregularity or deformity, and polished using 120- and 220-grit sandpapers (Miady, China) before they were considered ready for testing. A Chatillon® force measurement gauge was used with an MT Series manual testing stand (AMETEK®) to measure the peak tensile forces in the four groups. The ForceTest™ software (version 2.0, AMETEK®) was used to analyze the data measured by the force gauge. The results are exported and stored in Microsoft Excel for statistical analysis. Each sample was pulled vertically 12 times, and the tensile peak forces were recorded. The time taken to separate the blocks from the ball attachments (1.8 mm in diameter) was standardized to be 2.2 s. This corresponded to the normal speed of a denture moving away from the ridge during mastication (50 mm/min).[10,11]
Data were analyzed using the IBM® SPSS® Statistics software (version 25.0). The mean and standard deviation (SD) for each group were calculated. The Shapiro–Wilk test was used to assess the normality of the data [Table 1]. Levene’s test assessed the homogeneity of variance across groups, which turned out to be statistically significant (P < 0.05) [Table 2]. Further, analysis of variance (ANOVA) interaction effects was conducted using the Type III Sum of Squares [Table 3]. One-way ANOVA was used to determine whether there were any statistically significant differences (P < 0.05) between the means of the four groups, followed by Tukey post hoc tests to locate statistically significant differences (P < 0.05). The effect size of the mean differences between the groups was analyzed using the G*Power software (version 3.1.9.6). For all tests, P<0.05 is considered statistically significant. Visual illustrations were generated to illustrate the results. Cohen’s d was calculated to determine the effect sizes for the mean differences between the groups [Figure 2].
| Group | Statistic | df | Sig. |
|---|---|---|---|
| 0.0 | 0.983 | 48 | 0.688 |
| 1.5 | 0.933 | 48 | 0.009 |
| 3.0 | 0.953 | 48 | 0.055 |
| 4.5 | 0.943 | 48 | 0.022 |
P<0.05 is considered statistically significant
| F | df1 | df2 | P |
|---|---|---|---|
| 4.75 | 3.0 | 188.0 | 0.003 |
P<0.05 is considered statistically significant
| Sum of squares | df | Mean square |
F | P | |
|---|---|---|---|---|---|
| Between- group | 1060.530 | 3 | 353.510 | 562.51 | <0.001 |
| Within group | 118.150 | 188 | 0.628 | ||
| Total | 1178.679 | 191 |
P<0.05 is considered statistically significant
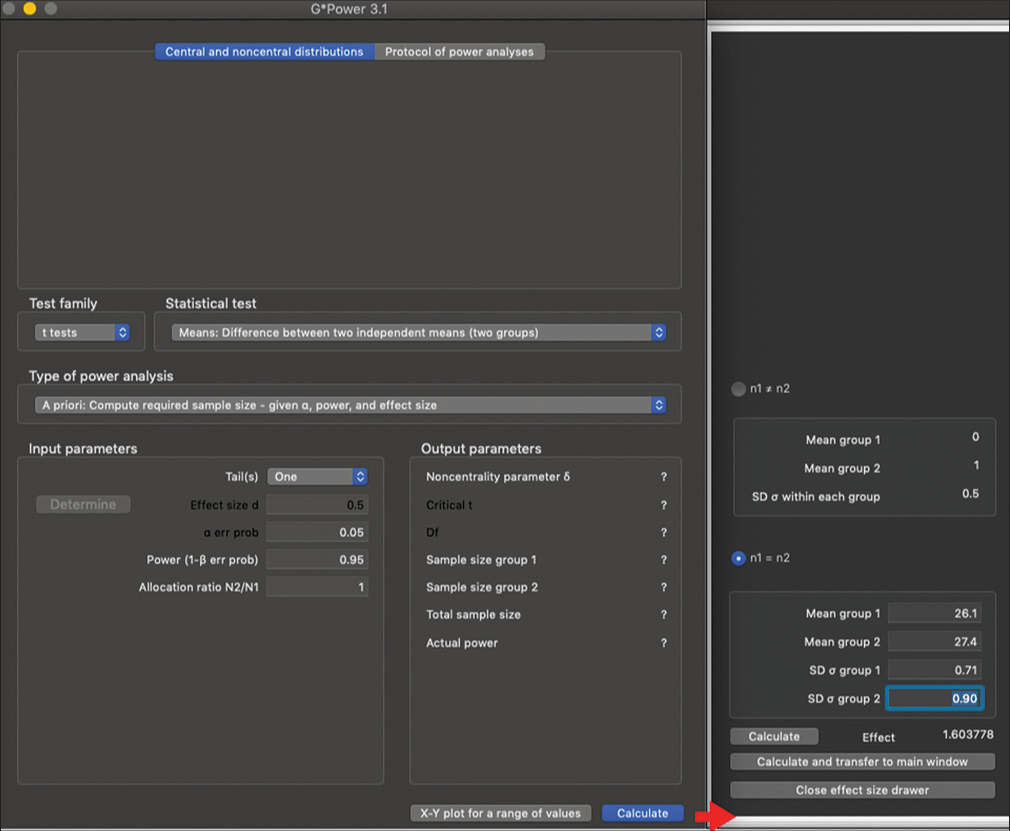
- Cohen’s d effect size between means.
RESULTS
One-way ANOVA showed statistically significant effects of IH on the mean retention force of the OD blocks. Group 0.0 mm had a greater mean retention force than the other groups (P<0.05). In addition, group 1.5 mm had a higher mean than groups 3.0 and 4.5 mm (P<0.05). However, the retention force for group 4.5 mm was slightly higher than group 3.0 mm (P<0.05). Groups 3.0 and 4.5 mm were at least two-fold less retentive than group 1.5 mm. A dramatic reduction in retention was found for any IH difference >1.5 mm. Figure 3 shows the mean retention force error bars for the four groups. Subsequent Tukey post hoc tests indicated that all the mean differences between groups were statistically significant, P < 0.05 [Table 3]. Despite its statistical significance, the mean difference between groups 3.0 and 4.5 mm expresses a negative value. The effect size for the difference between the 4.5 and 3.0 mm groups was the smallest (d = 1.60), and this may be too small to be of any clinical significance.
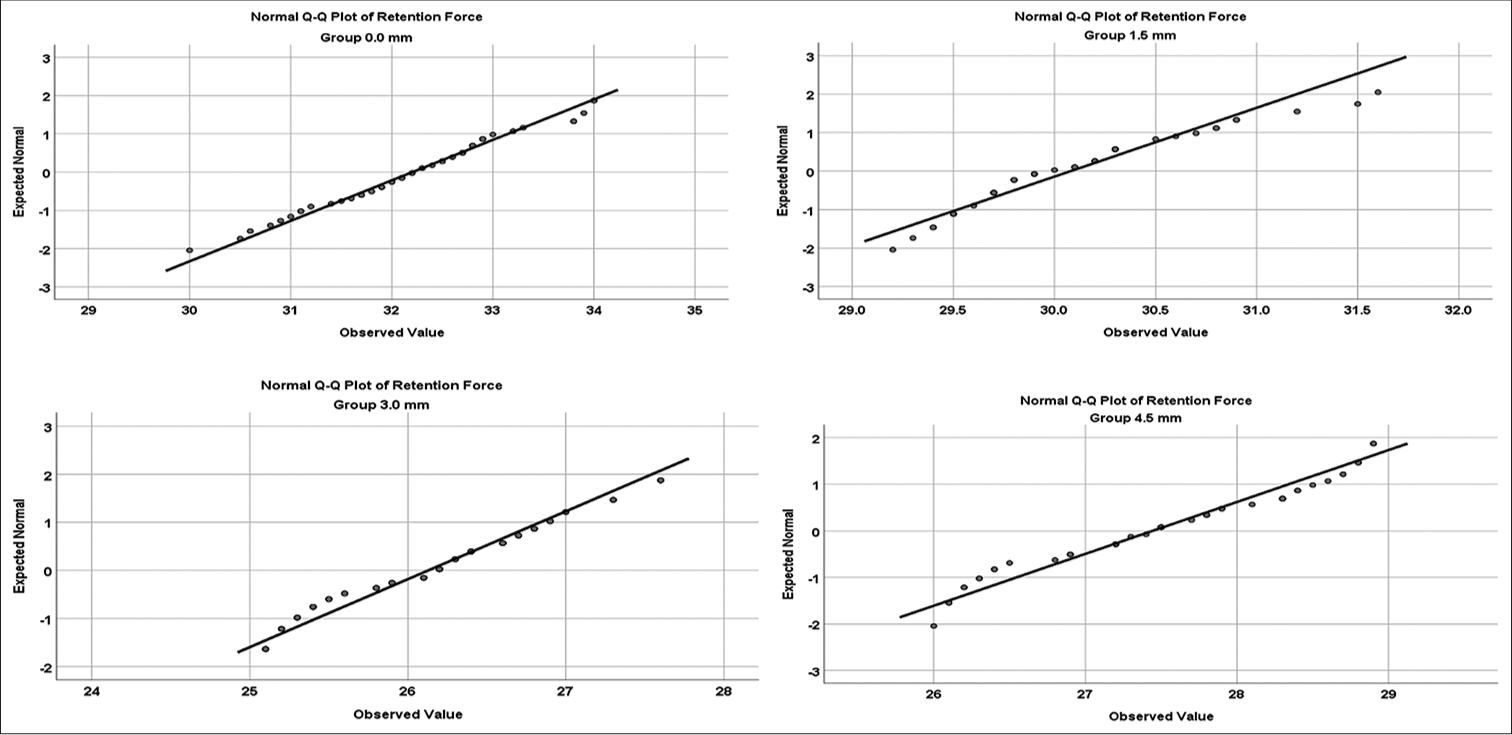
- Normal quantile plots for groups 0.0 mm, 1.5 mm, 3.0 mm, and 4.5 mm.
DISCUSSION
The results of this experiment reject the null hypothesis (H0) since statistically significant differences (P < 0.05) in retention means were found between evenly and unevenly placed MDIs retaining a lower OD. The retention mean of MDIs placed on the same level (32.2 ± 0.95 N) was significantly higher than the means of all other inter-implant levels (1.5 mm: 30.1 ± 0.56 N, 3.0 mm: 26.1 ± 0.71 N, 4.5 mm: 27.4 ± 0.90 N, P < 0.05). Over the past two decades, several studies have shown that ball abutments are among the most effective attachment systems in terms of OD retention.[12,13] The retention means of MDIs tested in this study across all inter-implant levels were at least five-fold higher than the minimum required force to stabilize an OD of 5 N.[14,15] One possible reason for this is the high level of technological advancements in the design and manufacturing of MDI Ball Abutments and Retentive Cap Inserts. The clear retentive caps used in this study were manufactured from a thick nylon layer by Rhein’83 (Italy) for Southern Implants© (the UK). The manufacturer believes that elastic retention provides superior and durable retention forces (up to 12 months). The mean retention force of group 0.0 mm (32.2 ± 0.95 N) was comparable to the mean values obtained at baseline in clinical studies (31.4 ± 8.3), which tested the retention of mandibular OD clinically on two SDIs with a ball attachment system.[16] Furthermore, most clinical studies have used four MDIs to retain a lower OD [7], whereas the results of this in vitro study showed that two MDIs placed parallel to the same level provided sufficient initial retention. The mean retention force of evenly placed MDIs was higher than that of Southern Implants© (UK), 1.8 kg (approximately 17.7 N). This could be because the company provided the retention force of a single MDI, which was expected to be less retentive than the two implants.[17] OD blocks retained by MDIs placed at a 1.5 mm height difference were 6.59% less retentive than those retained by MDIs at the same level (P < 0.05). This was the lowest effect of IH on OD block retention. The retention force of MDIs placed at 3.0 mm was 18.87% less retentive than those placed at the same level. This reduction in retention was three-fold greater than the 1.5 mm group. The results reveal an inverse correlation between the IH difference and the retention force of a lower OD.
However, the 4.5 mm group showed less reduction in retention force (14.78%) than the 3.0 mm group (18.87%) when compared to the MDIs placed on the same level. There was no clear explanation for group 4.5 mm being 4.09% more retentive than group 3.0 mm. The effect size (Cohen’s d) of similar in vitro studies was calculated and used as a reference point for evaluating the effect size between the groups’ 4.5 and 3.0 mm means. The calculated effect size between the two means was Cohen’s d = 1.4, which is comparable to the effect size between groups 4.5 and 3.0 mm (d = 1.6). The effect size between group 0.0 mm and 1.5 mm (d = 2.7), 3.0 mm (d = 7.3), and 4.5 mm (d = 5.2) was significantly higher than that between the groups 4.5 and 3.0 mm (d = 1.6). This suggested that the effect size between groups 4.5 and 3.0 mm was small and possibly clinically negligible. Although there is a lack of literature to support or reject these findings, it is well-documented that conventional CDs retained by a lower atrophic ridge are less retentive.[7,9] These studies tended to report the degree of ridge atrophy and ignored any irregularity in the ridge height, which has been found to contribute to a significant loss of OD retention. In this study, the reduction in OD retention is believed to be caused by the difference in the vertical position of the ball attachments on the uneven ridge form. The inter-attachment vertical height difference may have potentially altered the compression and return properties of Rhein’83 retentive plastic components. Furthermore, the affected plastic deformation and recoil properties, at some point during the retention tests, may have allowed one ball attachment to detach before the other. Although this was not observed, and if it were the case, it is well documented that one ball attachment is less retentive than two.[18] As a result, less force is required to pull one side of the OD and detach one ball attachment than to detach both attachments simultaneously. It appears that the greater the vertical inter-ID, the more likely it is that one abutment will detach before the other. Sia et al.,[19] in an in vitro study, observed the effect of different locator abutment heights and neglected to examine the impact of uneven ridges. Their results were significantly affected by the large surface area of tall locator abutments.
The dynamic phenomenon of one ball attachment detaching before the other was not observed in this in vitro study. If it had occurred at the microscopic level, the effect would have been minimal. This is because the OD block was retained by an exact matching ridge block, which allowed the MDIs to be detached simultaneously, with no implant standing out of the ridge block more than the others. The transmucosal part of the MDIs was not exposed and did not contribute to the retention force required to dislodge OD blocks. The results of this study suggest that MDIs with ball attachment systems should not be placed at an IH difference of more than 1.5 mm since an IH >1.5 mm dramatically compromises the retention forces of lower ODs. However, it is not always possible to avoid placing MDIs at different heights on atrophic and uneven ridges. Therefore, treatment options other than bone grafting should be explored. A simple treatment modality to overcome the loss of OD retention can be achieved by utilizing a more retentive plastic insert for MDIs placed in the lower portion of the uneven ridge. However, this approach cannot be confirmed unless further in vitro investigations are performed. Moreover, placing two MDIs at different angulations in the uneven RR may alter the OD retention force; the lower MDI can be distally angulated at 5° or 10°,[20] while the MDI at the higher ridge portion is placed straight. Clinical observation of a similar case, in which the lower implant was distally angulated [Figure 4], showed high initial OD retention and patient satisfaction. However, there was a rapid loss of retention and early detachment of the distally angulated lower implant ball attachment that had to be replaced due to wear, and the plastic retentive caps were replaced multiple times. Similar findings have been reported in an in vitro study.[21] Their results need to be interpreted with caution when applied to uneven RR because the retention loss and abutment wear pattern were assessed on a mandibular ridge model with a flat ridge form.
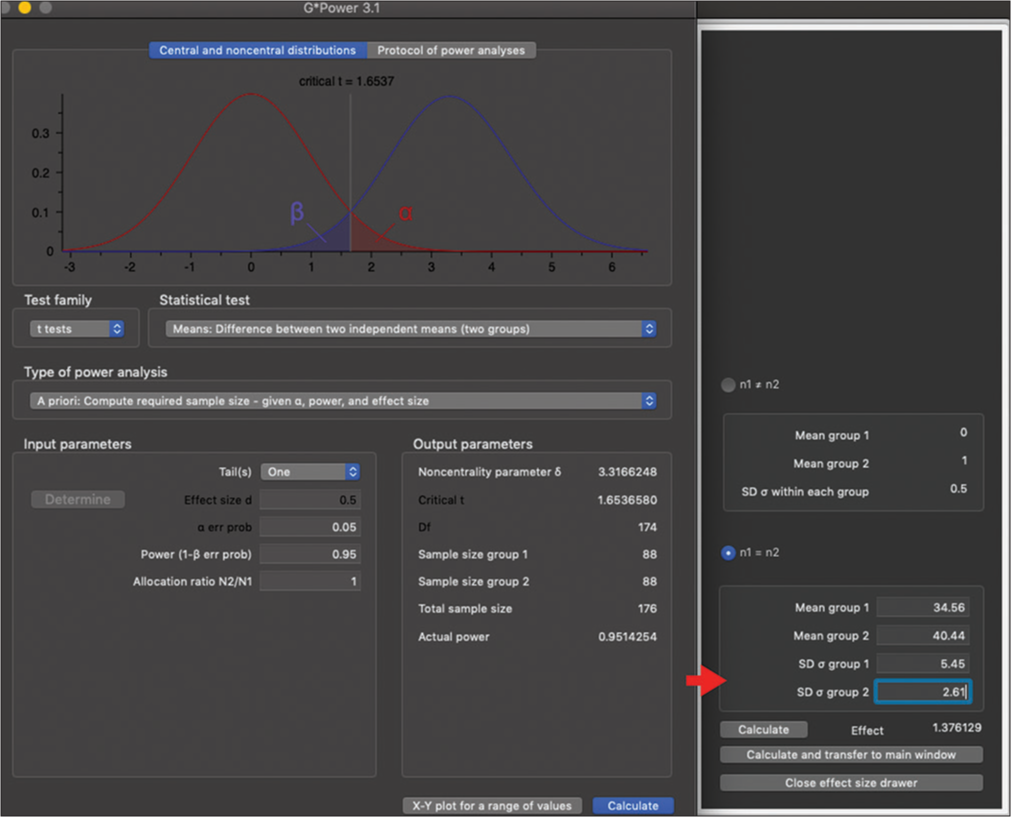
- Effect size calculation of a different study for comparison.
Another treatment option is to use a longer locator abutment to compensate for the lower portion of the uneven ridge. However, the actual clinical effect of this treatment is questionable. An approach similar to the all-on-four treatment modality[22] could be employed to gain support from the higher portion of the uneven ridge using SDIs. This was achieved by placing the implants in the lower part of the ridge at an angle toward the ridge portion with adequate height. An invasive treatment modality, but more predictable than grafting procedures, involves surgical reduction of the higher portion of the uneven ridge to reduce the inter-ridge height difference to ≤1.5 mm before placement of the MDIs. The lower the IH difference, the better the OD retention value; however, it is essential to weigh the desire to increase the OD retention force against the risk of further compromising the uneven atrophic ridge.
Limitations
This was a quantitative laboratory-based study conducted in a controlled environment; therefore, many clinical covariants were removed and not accounted for. The specimens were dry tested, and no artificial saliva was used to simulate the oral environment. In fatigue retention tests, the lack of a protective artificial salivary film on the ball attachment system may contribute to faster degradation of retentive plastic inserts.[23] The following factors play an important role in retention but were not considered: Adhesion, cohesion, interfacial surface tension, intimate tissue tension, border seal, and neuromuscular control.[24] The wear patterns of ball abutments and plastic retentive components have not been investigated, which is important to understand the effect of OD retention loss at the microscopic level.[22] Regardless of the high control of variables in this experiment, the manually controlled wheel in the testing stand may have introduced variability in the crosshead testing speed.[25]
CONCLUSION
Within the limitations of this in vitro study, the retention force of lower OD blocks was significantly affected by unevenly placed MDIs, with a dramatic decrease in retention observed for IH differences >1.5 mm.
Ethical approval
This lab-based study at the University of Manchester, classified as low-risk, has received ethical approval at the departmental level. https://www.manchester.ac.uk/research/environment/governance/ethics/approval/
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Implants purchased through funds from Manchester University.
References
- The continuing reduction of the residual alveolar ridges in complete denture wearers: A mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27:120-32.
- [CrossRef] [PubMed] [Google Scholar]
- Pattern of age related bone loss in mandibles. Eur J Oral Sci. 1980;88:134-46.
- [CrossRef] [PubMed] [Google Scholar]
- An alternative solution for a complex prosthodontic problem: A modified Andrews fixed dental prosthesis. J Prosth Dent. 2014;112:112-6.
- [CrossRef] [PubMed] [Google Scholar]
- Occlusal changes following posterior tooth loss in adults. Part 1: A study of clinical parameters associated with the extent and type of supraeruption in unopposed posterior teeth. J Prosthodont. 2007;16:485-94.
- [CrossRef] [PubMed] [Google Scholar]
- The McGill consensus statement on overdentures, Mandibular two-implant overdentures as first choice standard of care for edentulous patients. Montreal, Quebec, May 24-25, 2002. Int J Oral Maxillofac Implants. 2002;17:601-2.
- [Google Scholar]
- Mandibular two implant-supported overdentures as the first choice standard of care for edentulous patients-the York Consensus Statement. Br Dent J. 2009;207:185-6.
- [CrossRef] [PubMed] [Google Scholar]
- A pilot randomised controlled trial evaluating mini and conventional implant retained dentures on the function and quality of life of patients with an edentulous mandible. BMC Oral Health. 2017;17:53.
- [CrossRef] [PubMed] [Google Scholar]
- Mini-dental implant insertion with the auto-advance technique for ongoing applications. J Oral Implantol. 2001;27:32-37.
- [CrossRef] [PubMed] [Google Scholar]
- One-year clinical outcomes of locking taper Equator attachments retaining mandibular overdentures to narrow diameter implants. Clin Implant Dent Relat Res. 2018;20:483-92.
- [CrossRef] [PubMed] [Google Scholar]
- The influence of interimplant distance and attachment type on the retention characteristics of mandibular overdentures on 2 implants: Initial retention values. Int J Prosthodont. 2006;19:507-12.
- [Google Scholar]
- The efficiency of cobalt samarium (Co5Sm) magnets as retention units for overdentures. J Dent. 1983;11:324-33.
- [CrossRef] [PubMed] [Google Scholar]
- Maximum dislodging forces of implant overdenture stud attachments. Int J Oral Maxillofac Implants. 2002;17:526-35.
- [Google Scholar]
- Retention and stability of overdentures with ball, bar, or magnet attachments: A systematic review. Drug Invent Today. 2018;10:723-7.
- [Google Scholar]
- In vitro retention force changes of prefabricated attachments for overdentures. J Oral Rehabil. 2003;30:671-8.
- [CrossRef] [PubMed] [Google Scholar]
- The service life of implant-retained overdenture attachment systems. J Prosthet Dent. 2009;102:74-80.
- [CrossRef] [PubMed] [Google Scholar]
- Retention and postinsertion maintenance of bar-clip, ball and magnet attachments in mandibular implant overdenture treatment: An in vivo comparison after 3 months of function. Clin Oral Implants Res. 2003;14:720-6.
- [CrossRef] [PubMed] [Google Scholar]
- Clinical outcome of removable prostheses supported by mini dental implants: A systematic review. Acta Odontol Scand. 2018;76:628-37.
- [CrossRef] [PubMed] [Google Scholar]
- Impact of single implant versus two-implant mandibular retained overdentures on retention and success rate in totally edentulous patients: A randomized controlled clinical trial. J Osseointegration. 2018;10:79-86.
- [Google Scholar]
- Effect of locator abutment height on the retentive values of pink locator attachments: An in vitro study. J Prosthet Dent. 2017;117:283-8.
- [CrossRef] [PubMed] [Google Scholar]
- The in vitro effect of different implant angulations and cyclic dislodgement on the retentive properties of an overdenture attachment system. J Prosthet Dent. 2009;102:140-7.
- [CrossRef] [PubMed] [Google Scholar]
- Retention and wear behaviors of two implant overdenture stud-type attachments at different implant angulations. J Prosth Dent. 2017;117:628-35.
- [CrossRef] [PubMed] [Google Scholar]
- The All-on-4 treatment concept for the rehabilitation of the completely edentulous mandible: A longitudinal study with 10 to 18 years of follow-up. Clin Implant Dent Relat Res. 2019;21:565-77.
- [CrossRef] [Google Scholar]
- Evaluation of stable retentive properties of overdenture attachments. Stomatologija. 2005;7:115-20.
- [Google Scholar]
- A contemporary review of the factors involved in complete dentures. Part III: Support. J Prosthet Dent. 1983;49:306-13.
- [CrossRef] [PubMed] [Google Scholar]
- Testing the retention of attachments for implant overdentures-validation of an original force measurement system. J Oral Rehabil. 2010;37:54-62.
- [CrossRef] [PubMed] [Google Scholar]






